Doctors Who SWAG – The Harmful Impact of Guessing for Disability & Workers’ Compensation Patients
For many worker’s compensation or disability patients, their primary care doctor is the go-to to treat and diagnose their injuries. However, few family physicians are trained to determine a patient’s ability to work – despite being asked to do so repeatedly.
Too often, I’ve heard stories of doctors who SWAGGED (took a scientific wild a** guess) at a patient’s capacity for work without testing. While this SWAG is based on the doctor’s knowledge of the patient’s injuries, guessing at function without testing to confirm it is akin to throwing out a broken lamp without first testing the light bulb to ensure it’s working. And it can have devastating consequences for patients.
Over the years, I’ve done thousands of Functional Capacity Evaluations, or FCEs, but there’s one in particular that I’ll never forget.
Meet Bob, a Plumber
Bob was a 50-something male who had suffered a compression fracture of his thoracic spine eight years prior. If you’re not familiar with the term, a compression fracture is when a bone in the spine fractures or dissolves. This is a common injury caused by falls or other traumatic injuries.
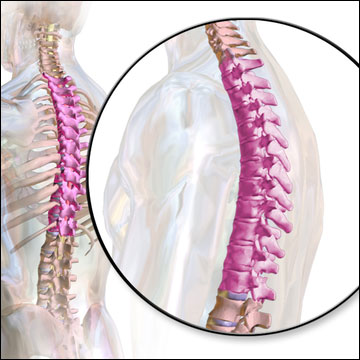 In Bob’s case, the damage was to the thoracic area, located in the middle of the spine. After surgery and extensive physical rehabilitation, he was declared maximum medically improved with permanent restrictions.
In Bob’s case, the damage was to the thoracic area, located in the middle of the spine. After surgery and extensive physical rehabilitation, he was declared maximum medically improved with permanent restrictions.
The problem here is that Bob was never tested; rather his physician gave him a note stating he should not lift more than 20 lbs. The note had no timeline or follow up scheduled. Bob literally folded up the note, placed it in his wallet, and ceased working as a plumber – his career of nearly 25 years.
For the subsequent eight years, Bob worked as a cashier. By the time he came to me, Bob was barely able to keep afloat and was basically starving. He’d just applied for SSDI and vocational assistance and needed to be evaluated as part of his claim.
The Functional Test Yielded Surprising Results
The functional testing revealed that Bob could safely lift 50 lbs. Based on a reasonable degree of medical and ergonomic certainty, the testing showed that he could have likely worked as a plumber all along.
This is a stark lesson to all medical, vocational, and human resources professionals. The advantages of going the extra step and using objective functional testing to assess function and fitness-for-duty cannot be overstated.
In Bob’s case, a referral for an FCE could have circumvented years of missed wages and distress.
Research supports that job-specific testing is superior to functional estimates by a physician.
The well-known research study Comparing self-report, clinical examination and functional testing in the assessment of work-related limitations in patients with chronic low back pain (Brouwer et al., 2009) showed the importance of functional testing. Researchers concluded that the limitations derived from physicians’ clinical examination were higher than those derived from Functional Capacity Evaluation.
With our clients’ lives and livelihoods at risk, I strongly advocate objective functional and fitness-for-duty testing. Not because it is my line of work; it’s simply the right thing to do. Ethically and legally, we medical, vocational and human resources professionals owe it to our clients to not cut corners when assessing function and fitness-for-duty.
When objective testing is performed, the results provide evidence-based information on which stakeholders can rely to place a worker into a specific job, or at least, to specific job tasks.

References
Brouwer, S., Dijkstra, P. U., Stewart, R. E., Göeken, L. N., Groothhoff, J. W., & Geertzen, J. H. (2009, 7). Comparing self-report, clinical examination and functional testing in the assessment of work-related limitations in patients with chronic low back pain. Retrieved from Northern Centre for Health Care Research, University Medical Centre Groningen, University of Groningen, Groningen, The Netherlands website: https://www.tandfonline.com/doi/abs/10.1080/09638280500052823
Related Posts